 Over the years, magnetic resonance imaging (MRI) emerged as a powerful imaging modality to detect cartilage lesions and structural changes of the hip joint. For decades, conventional radiography (CR) has been used to support the clinical diagnosis of hip OA. 
In patients with clinically suspected hip OA, medical imaging contributes to confirm the diagnosis and rule out alternative diagnoses by demonstrating cartilage lesions and associated structural changes. Hip osteoarthritis (OA) is a highly prevalent and disabling disorder that affects elderly but also young patients with a high socio-economic burden. The absence of a validated MR biomarker of early OA, together with issues related to machine availability and MRI protocol repeatability, prevent the widespread use of MRI in clinical trials. MRI seems to be more suitable than radiographs as a biomarker for clinical trials addressing early OA. 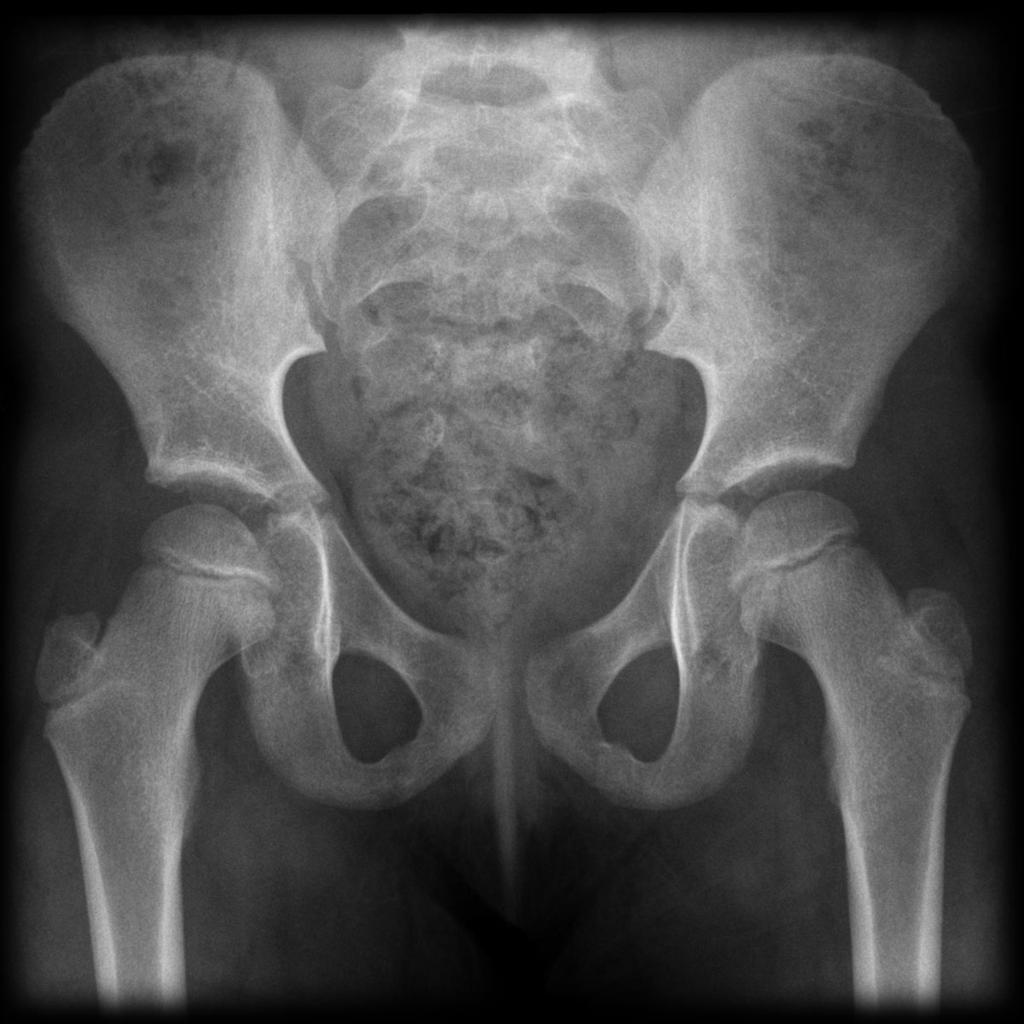
However, structural joint changes are frequent in asymptomatic population and neither radiographs nor MRI have shown a good correlation with pain and functional impairment. Magnetic resonance imaging (MRI) is more sensitive to detect joint effusion/synovitis, cartilage, labral, and bone marrow lesions. The choice of the appropriate lateral view depends on the clinical indication, Lequesne’s false profile being valuable in the assessment of OA. They should be obtained in a rigorous technique that includes an antero-posterior (AP) radiograph of the pelvis. Conventional radiographs are recommended as the first line imaging modality to investigate chronic hip pain. Diagnosis of hip osteoarthritis (OA) is based on clinical arguments, and medical imaging is obtained to confirm the diagnosis and rule out other possible sources of pain. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
